Sex, Gender, & Intersectional Analysis
Case Studies
- Science
- Health & Medicine
- Chronic Pain
- Colorectal Cancer
- Covid-19
- De-Gendering the Knee
- Dietary Assessment Method
- Gendered-Related Variables
- Heart Disease in Diverse Populations
- Medical Technology
- Nanomedicine
- Nanotechnology-Based Screening for HPV
- Nutrigenomics
- Osteoporosis Research in Men
- Prescription Drugs
- Systems Biology
- Engineering
- Assistive Technologies for the Elderly
- Domestic Robots
- Extended Virtual Reality
- Facial Recognition
- Gendering Social Robots
- Haptic Technology
- HIV Microbicides
- Inclusive Crash Test Dummies
- Human Thorax Model
- Machine Learning
- Machine Translation
- Making Machines Talk
- Video Games
- Virtual Assistants and Chatbots
- Environment
Heart Disease in Diverse Populations: Analyzing Sex and Gender
The Challenge
Ischemic heart disease (IHD) is the number one killer of U.S. and European populations (WHO, 2008). Nonetheless heart disease has been defined as primarily a male disease, and “evidence-based” clinical standards have been created based on male pathophysiology and outcomes. As a result, women and gender-diverse individuals are often mis- and under-diagnosed (EUGenMed et al. 2016; Taylor et al., 2011).
Method: Analyzing Gender in Health & Biomedicine
Transnational tobacco companies’ advertisements have long linked smoking to sexiness, thinness, intelligence, modernity, and liberation, a tactic increasingly deployed in developing countries (SRITA). Analyzing gender can help consumers understand how tobacco advertising plays on popular images of femininity and masculinity to sell a product. Banning the manufacture and sale of cigarettes, combined with efforts to de-romanticize smoking in movies, television, and other media, can help prevent this disease (Proctor, 2011; Hawkes & Buse, 2018).
Gendered Innovations:
Research on heart disease offers one of the most developed examples of gendered innovations. From the expanding literature on sex and gender analysis in this area, we highlight several key developments:
- 1. Redefining the Pathophysiology of Myocardial Ischemia: Analyzing sex in clinical research has led to an understanding that heart disease in women often has a different pathophysiology than in men—particularly in younger adults.
- 2. Developing New Diagnostic Techniques: New Diagnostic techniques—some still experimental—are more effective than angiography for understanding the causes of ischemic heart disease (IHD) in women with chest pain in the absence of obstructive coronary artery disease (CAD).
- 3. Understanding Sex Differences in Symptoms has led to earlier and better diagnosis of IHD in women.
- 4. Analyzing Gender in Risk Factors and Prevention reveals that smoking has historically been far more common among men than women; however, in many countries smoking rates are increasing among women due to targeted marketing by tobacco companies (Hawkes &. Buse, 2018).
- 5. Understanding Gender Independent of Biological Sex: Gender, independent of sex, predicts poor outcomes of acute coronary syndrome in both women and men. Individuals with high feminine gender scores were twice as likely to be re-admitted to hospital and to experience worse prognosis following discharge after heart attack (Hunt et al. 2007; Pelletier et al., 2016; Nielsen et al., 2020).
- 6. Mitigating Bias in Care Pathways for Heart Disease: Emergency room protocols that eliminate gender bias in ST-elevation heart attack diagnosis reduce the mortality gap for women by accelerating access to coronary angiography (Huded et al. 2018).
- 7. Studying Cardiovascular Health in Transgender Individuals undergoing Gender-Affirming Therapies is not only mandatory to improve healthcare options, but also allows a deeper understanding of the role of sex hormones in cardiovascular health in adult bodies.
Gendered Innovation 1: Redefining the Pathophysiology of Myocardial Ischemia
Gendered Innovation 2: New Diagnostic Techniques
Gendered Innovation 3: Understanding Sex Differences in Symptoms
Gendered Innovation 4: Gender Analysis in Risk Factors and Prevention
Gendered Innovation 5: Importance of Gender Independent of Biological Sex
Gendered Innovation 6: Mitigating Bias in Care Pathways for Heart Disease
Gendered Innovation 7: Studying Cardiovascular Health in Transgender Individuals undergoing Gender-Affirming Therapies
Conclusions
Next Steps
The Challenge
Heart disease has been considered primarily a male disease. This perception may exist because myocardial infarction (MI) manifests about ten years later in women than in men. Nonetheless, ischemic heart disease (IHD) is the major killer of all individuals regardless of their gender (WHO, 2008). Now, after thirty years of research, heart disease offers one of the most developed examples of gendered innovations. Sex and gender analysis prompted policy changes, increased the representation of women and gender-diverse subjects in heart disease research, and enhanced knowledge about how biological sex and gender behaviors influence heart disease. Results include improved diagnosis and treatment in women and men alike, a growing body of knowledge about the cardiovascular health of transgender persons as well as prevention campaigns that utilize an understanding of gender to promote heart-healthy behaviors and target risk behaviors.
Gendered Innovation 1: Redefining the Pathophysiology of Myocardial Ischemia
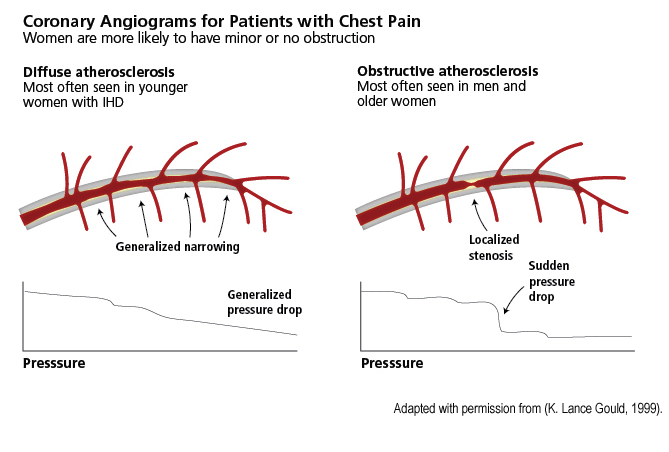
The pathophysiology underlying myocardial ischemia often differs between women and men (Bairey Merz et al., 2010). Coronary angiography, the "gold standard" for diagnosing patients with angina (chest pain), typically results in a diagnosis of obstructive coronary artery disease (CAD) in men (see chart below, right), but frequently fails to identify the cause in a large proportion of women (Shaw et al., 2009; Bugiardini et al., 2005). As a result, many women with chest pain, but “normal” angiograms (see chart below, left), are under- and mis-diagnosed and treated. Many women with angina are told that they have no significant heart disease.
New studies show, however, that the prognosis for these women is not benign: Women with a primary diagnosis of “non-specific chest pain” may suffer heart attack or stroke shortly after being discharged from hospitals (Robinson et al., 2008). This may also be true for men with angina and non-obstructive CAD. Large-scale randomized trials are needed to better understand the pathophysiology and optimal therapies for women and men with angina and “normal” angiograms (Shaw et al., 2009).
Large-scale studies have found that coronary angiography is often ineffective in diagnosing heart disease in women because it images disease in large but not small coronary vessels. The U.S. National Heart, Lung, and Blood Institute’s Women’s Ischemic Syndrome Evaluation (WISE) used innovative diagnostic tests and techniques (selected to obviate difficulties relevant to women, such as breast imaging artifact) to examine women who experienced chest pain but did not have obstructive CAD (Bairey Merz et al., 1999). These women are more frequently affected by modifications of the small vessels of the heart (microvascular disease). Microvascular disease is caused by damaged vessel linings (endothelial dysfunction), inappropriate constriction (coronary vasospasm), malfunctions in the small vascular branches (microvascular dysfunction), or squeezing from overlying heart muscle (myocardial bridging). These changes may lead to the same symptoms as traditional obstructive disease.
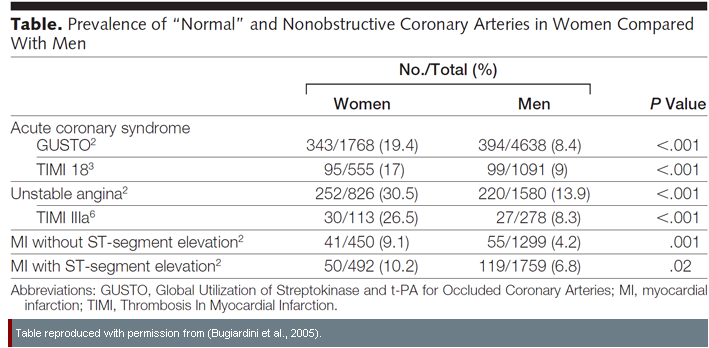
New research also suggests that “ischemic heart disease” (IHD) may better describe women’s underlying disease than obstructive CAD or coronary heart disease (CHD) (Shaw et al., 2009). Given that in women the affected vessels are frequently not well represented on traditional angiograms, women’s coronary angiograms are more likely than men’s to be classified as “normal” or “nonobstructive” (i.e., open coronary arteries) despite the presence of unstable angina, acute coronary syndrome, or other coronary conditions—see table below:
Method: Analyzing Sex in Biomedicine
To interpret sex-specific physiology, disease, and outcomes, data must be collected and analyzed by sex. The WISE study evaluated only women, yet has been cited as evidence of sex differences in pathophysiology. To determine sex differences, sufficient numbers of both women and men are needed, and samples should be matched or data should be adjusted to control for potential confounding factors, such as age, reproductive status, socioeconomic status, body composition, protective and risk behaviors, etc. (see Designing Health and Biomedical Research).
Gendered Innovation 2: New Diagnostic Techniques
Coronary angiography is widely considered the “gold standard” for evaluating coronary heart disease. Angiography, however, can cause hematomas and other bleeding complications; these occur more often in women patients than men patients (Berry et al., 2004). Gendered innovations in diagnosis include new angiography procedures—such as entry through the radial artery—which reduce bleeding complications (Cantor et al., 2007). These innovations, especially important to women patients, can also benefit men patients.
Important future gendered innovations will include new diagnostic techniques that provide evidence of pathophysiologic causes of myocardial ischemia in individuals with chest pain but no obstructive CAD—and who are at risk for subsequent MI or unstable angina. These include:
- ● Coronary reactivity testing (von Mering et al., 2004; Pepine et al., 2010).
● Intravascular ultrasound (IVUS) (Khuddus et al., 2010).
● Cardiac magnetic resonance imaging (MRI) and cardiac spectroscopy (Ishimori et al., 2011; Buchthal et al., 2000).
● Advanced radionuclide imaging including positron emission tomography (PET) (Johnson et al., 2011).
● Perfusion stress echocardiography (Kaul, 2011).
Gendered Innovation 3: Understanding Sex Differences in Symptoms
Understanding symptoms of acute coronary syndrome (ACS) is critical to optimizing treatment and outcomes. An international study of 26,755 patients (29% women) with ACS found that “chest pain was the most common symptom for both men (94%) and women (92%)” (Dey et al., 2009). A study examining more than 1 million patients who had experienced a heart attack, however, demonstrated that especially young women frequently have no symptoms when suffering from a heart attack or experience nausea, dizziness, shortness of breath rather than chest pain (Canto et al., 2012). In the past, these symptoms were classified as “atypical”; today doctors recognize them as valid presentations of symptoms for heart disease (Ibanez et al., 2018).
Gendered Innovation 4: Gender Analysis in Risk Factors and Prevention
Most risk factors for IHD (e.g., older age, adverse lipoprotein profiles, high blood pressure, high blood glucose, diabetes, smoking, obesity, physical inactivity, and high fat diets) apply to both women and men. However, there are differences in the prevalence and adverse impact of these risk factors (Mosca et al., 2012).
Smoking, for example, has historically been far more common among men than women; about 7.5% of the world’s tobacco smokers are women (WHO, 2010a). Overall, cigarette smoking is declining among women in the U.S.,Western Europe, and other industrialized nations but is either stable or increasing in Southern, Central, and Eastern Europe, and many parts of the developing world (WHO, 2010b) due to targeted gender-specific marketing efforts in these regions (WHO, 2018).
Smoking is the major preventable cause of death in the U.S. and Europe, and is a major risk factor for heart attack and stroke (Shafey et al., 2009; Millet et al., 2018). Of all the traditional risk factors, smoking and diabetes mellitus have been demonstrated to be the greatest (Peters et al., 2013; Peters et al., 2014).Method: Analyzing Gender in Health & Biomedicine
Transnational tobacco companies’ advertisements have long linked smoking to sexiness, intelligence, liberation, thinness, and modernity, a tactic increasingly deployed in developing countries (SRITA). Analyzing gender can help consumers understand how tobacco advertising plays on popular images of femininity and masculinity to sell a product. Banning the manufacture and sale of cigarettes, combined with efforts to de-romanticize smoking in movies, television, and other media, can help prevent this disease (Proctor, 2011; Hawkes & Buse, 2018).
Gendered Innovation 5: Importance of Gender Independent of Biological Sex
 Hunt et al. (2007) and Pelletier et al. (2016) revealed that gender, independent of sex, predicts poor outcomes of acute coronary syndrome in both women and men. Individuals with high feminine gender scores were twice as likely to be re-admitted to hospital and to experience worse prognosis following discharge after heart attack. The mechanism underlying this observation is currently under study and may be linked to cortisol and chronically high stress levels. For gender-related variables for health research, see (Nielsen et. al., 2020).
Hunt et al. (2007) and Pelletier et al. (2016) revealed that gender, independent of sex, predicts poor outcomes of acute coronary syndrome in both women and men. Individuals with high feminine gender scores were twice as likely to be re-admitted to hospital and to experience worse prognosis following discharge after heart attack. The mechanism underlying this observation is currently under study and may be linked to cortisol and chronically high stress levels. For gender-related variables for health research, see (Nielsen et. al., 2020).
Gendered Innovation 6: Mitigating Bias in Care Pathways for Heart Disease
To reduce the gender mortality gap often due to delayed diagnosis, an emergency department in the Cleveland Clinic, Cleveland, Ohio, implemented a 4-step gender-neutral protocol to manage individuals with suspected ST-segment elevation myocardial infarction (STEMI). Prior to implementation of the protocol, when a STEMI patient came to the hospital, the decision to refer the patient to the cardiac catheterization lab was made jointly between the emergency department physician, the on-call cardiology fellow, and the cardiac catheterization lab physician. Whether the patient received guideline-directed medical therapy (defined as the administration of aspirin, a P2Y12 inhibitor, and an anticoagulant) depended on the preferences of individual physicians. In the catheterization lab, the choice of radial or femoral vascular access was made by the individual operator.
The 4-step protocol included four changes. First, the emergency department physician did not need to consult with cardiology before activating the catheterization lab. Second, the triage of STEMI patients was standardized by using a “STEMI Safe Handoff Checklist” that outlined roles for the physicians and nurses, provided guidance on guideline-directed medical therapy, and informed the catheterization lab of risk factors. Third, patients were transferred to an available catheterization lab immediately. Finally, the hospital encouraged the use of the radial artery in patients without contraindications. <
The 4-step process improved sex disparities in the use of guideline-directed medical therapy, median door-to-balloon time, in-hospital adverse events, and 30-day mortality rates. The absolute sex difference in 30-day mortality decreased from 6% to 3%, providing evidence that a systems-based approach to STEMI care reduces sex disparities and improves outcomes in women (Huded et al., 2018).
Gendered Innovation 7: Cardiovascular Health for Transgender Individuals
Many transgender individuals seek hormone therapy in order to bring their bodies more in line with their gender identities. Hormone therapy involves either estrogens (sometimes in combination with androgen blockers) or androgens. The hormones are given at a higher dosage than previously studied (for example, for contraceptives or hormone therapy in postmenopausal women) and may increase a patient’s cardiovascular risk.
Hormonal therapy changes the blood lipid profiles of the user (Maraka et al., 2017) in ways not fully predictable from studying cisgender individuals (i.e., individuals for whom sex assigned at birth matches their current gender identity). Transwomen often take estrogens at levels associated with an increased risk of venous thromboembolism (venous clots, most frequently in the large veins of the leg) and a slightly increased risk of heart attacks (Irwig, 2018). Including transgender individuals in clinical studies is important to allow for better risk prediction and care (Rytz, et al., 2023). This will also result in better understandings of high-dosage hormones on cardiovascular health in adults overall.
Conclusions
Sex analysis in the context of heart disease research has revealed clinically significant differences in pathophysiology between women and men. Awareness of these sex differences has guided the development of new diagnostics, such as measurement of coronary flow reserve. Combating tobacco smoking has required both gender analysis and sex analysis: gender roles influence women, men, and gender-diverse individual’s patterns of tobacco usage, while biological sex differences affect women’s and men’s susceptibility to smoking-related heart disease. Gender, independent of sex, predicts poor outcomes of acute coronary syndrome in both women and men. Including transgender individuals taking hormonal therapy in clinical trials represents an opportunity for more inclusive care and a chance to learn about the effects of high-dose hormones on cardiovascular health in adult bodies.
Next Steps
- 1. WHO has called for research to systematically “incorporate attention to sex and gender in design, analysis, and interpretation of findings.” WHO also recommends increasing the number of older women in clinical trials in order to establish both sex- and age-specific guidelines for treatment (WHO, 2009).
- 2. Since the 1980s, the U.S. NIH and the FDA have encouraged the inclusion of women and minorities in all federally funded research. Recent data demonstrate that women are currently well-represented in clinical trials for atrial fibrillation and hypertension, yet are still significantly under-represented in trials for coronary heart disease and heart failure (Scott et al., 2018).
- 3. In 2005, the European Society of Cardiology launched its Women at Heart initiative, with the aim of closing “a disturbing gap in the knowledge, understanding, and general awareness of cardiovascular disease in women, across medical audiences as a whole.” The primary goal of Women at Heart is to improve medical professionals’ handling of women at risk for cardiovascular diseases (European Society of Cardiology, 2011). In the last decade, female-predominant forms of disease, such as microvascular disease, as well as female-specific risk factors, such as pregnancy complications, are moving into the focus of research.
- 4. Given recent reports of the potentially increased risk of heart disease in transgender individuals (Alzahrani et al., 2019; Nota et al., 2019), substantial research is needed to confirm these risks and develop appropriate guidelines for prevention.
Works Cited
Alzahrani, T., Nguyen, T., Ryan, A., Dwairy, A., McCaffrey, J., Yunus, R., ... & Reiner, J. (2019). Cardiovascular disease risk factors and myocardial infarction in the transgender population. Circulation: Cardiovascular Quality and Outcomes, 12(4). https://doi.org/10.1161/CIRCOUTCOMES.119.005597
Bairey Merz, C., Mark, S. Boyan, B., Jacoba, A., Shah, P., Shaw, L., Taylor, D., & Marbán, E. (2010). Proceedings from the Scientific Symposium: Sex Differences in Cardiovascular Disease and Implications for Therapies. Journal of Women's Health, 19 (6), 1059-1072.
Bairey Merz, C., Shaw, L., Reis, S., Bittner, V., Kelsey, S., Olson, M., Johnson, B., Pepine, C., Mankad, S., Sharaf, B., Rogers, W., Pohost, G., Lerman, A., Quyyumi, A., & Sopko, G. (2006). Insights from the National Heart, Lung, and Blood (NHLBI)-Sponsored Women’s Ischemia Syndrome Evaluation (WISE) Study, Part II: Gender Differences in Presentation, Diagnosis, and Outcome with Regard to Gender-Based Pathophysiology of Atherosclerosis and Macrovascular and Microvascular Coronary Disease. Journal of the American College of Cardiology, 47 (3), S21-S29.
Bairey Merz, C., Kelsey, S., Pepine, C., Reichek, N., Reis, S., Rogers, W., Sharaf, B., & Sopko, G. (1999). The Women’s Ischemia Syndome Evaluation (WISE) Study: Protocol Design, Methodology, and Feasibility Report. Journal of the American College of Cardiology, 33 (6), 1453-1461.
Berry, C., Kelly, J., Cobbe, S., & Eteiba, H. (2004). Comparison of Femoral Bleeding Complications after Coronary Angiography versus Percutaneous Coronary Intervention. American Journal of Cardiology, 94 (3), 361-363.
Buchthal, S., den Hollander, J., Bairey Merz, C., Rogers, W., Pepine, C., Reichek, N., Sharaf, B., Reis, S., Kelsey, S., & Pohost, G. (2000). Abnormal Myocardial Phosphorus-31 Nuclear Magnetic Resonance Spectroscopy in Women with Chest Pain but Normal Coronary Angiograms. New England Journal of Medicine, 342 (12), 829-835.
Bugiardini, R., & Bairey Merz, C. (2005). Angina with “Normal” Coronary Arteries: A Changing Philosophy. Journal of the American Medical Association 293 (4), 477-484.
Cantor, W., Mahaffey, K., Huang, Z., Das, P., Gulba, D., Glezer, S., Gallo, R., Ducas, J., Cohen, M., Antman, E., Langer, A., Kleiman, N., White, H., Chisholm, R., Harrington, R., Ferguson, J., Califf, R., & Goodman, S. (2007). Bleeding Complications in Patients with Acute Coronary Syndrome Undergoing Early Invasive Management can be reduced with Radial Access, Smaller Sheath Sizes, and Timely Sheath Removal. Catheterization and Cardiovascular Interventions, 69 (1), 73-83.
Chen, W., Woods, S., & Puntillo, K. (2005). Gender Differences in Symptoms Associated with Acute Myocardial Infarction: A Review of the Research. Heart and Lung: The Journal of Acute and Critical Care, 34 (4), 240-247.
Dey, S., Flather, M., Devlin, G., Brieger, D., Gurfinkel, E., Steg, P., Fitzgerald, G., Jackson, E., & Eagle, K. (2009). Sex-Related Differences in the Presentation, Treatment, and Outcomes among Patients with Acute Coronary Syndromes: The Global Registry of Acute Coronary Events. Heart, 95 (1), 20-26.
EUGenMed Cardiovascular Clinical Study Group, Regitz-Zagrosek, V., Oertelt-Prigione, S., Prescott, E., Franconi, F., Gerdts, E., Foryst-Ludwig, A., Maas, A. H., Kautzky-Willer, A., Knappe-Wegner, D., Kintscher, U., Ladwig, K. H., Schenck-Gustafsson, K., & Stangl, V. (2016). Gender in cardiovascular diseases; impact on clinical manifestations, management, and outcomes. European Heart Journal, 37(1), 24-34.
European Medicines Agency (EMEA). (2006). Committee for Medicinal Products for Human Use (CHMP) Reflection Paper on Gender Differences in Cardiovascular Diseases. London: EMEA.
European Society of Cardiology (ESC). (2011). Women at Heart: Scientific Material.
Hawkes, S., & Buse, K. (2018). Gender-Responsive Tobacco Control: Evidence and Options for Policies and Programmes. . World Health Organization Framework Convention on Tobacco Control.
Huded, C. P., Johnson, M., Kravtiz, K., Menon, V., Abdallah, M., Gullett, T. C., … Khot, U. N. (2018). 4-Step Protocol for Disparities in STEMI Care and Outcomes in Women. Journal of the American College of Cardiology 71 (19), 2122-2132.
Hunt, K., Lewars, H., Emslie, C., & Batty, G. D. (2007). Decreased risk of death from coronary heart disease amongst men with higher ‘femininity’scores: a general population cohort study. International Journal of Epidemiology, 36(3), 612-620.
Ibanez, B., James, S., Agewall, S., Antunes, M. J., Bucciarelli-Ducci, C., Bueno, H., … Widimský, P. (2018). 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation: The Task Force for the management of acute myocardial infarction in patients presenting with ST-segment elevation of the European Society of Cardiology (ESC). European Heart Journal 39 (2), 119-177.
Irwig, M. S. (2018). Cardiovascular Health in Transgender People. Reviews in Endocrine and Metabolic Disorders, 19 (3), 243-251.
Ishimori, M., Martin, R., Berman, D., Goykhman, P., Shaw, L., Shufelt, C., Slomka, P., Thomson, L., Schapira, J., Yang, Y., Wallace, D., Weisman, M., & Bairey Merz, C. (2011). Myocardial Ischemia in the Absence of Obstructive Coronary Artery Disease in Systemic Lupus Erythematosus. Journal of the American College of Cardiology: Imaging, 4 (1), 27-33.
Johnson, N., & Gould, K. (2011). Positron Emission Tomography. In Thompson, P. (Ed.), Coronary Care Manual 2E, pp. 179-186. Chatswood: Elsevier Australia.
Khuddus, M., Pepine, C., Handberg, E., Bairey Merz, C., Sopko, G., Bavry, A., Denardo, S., McGorray, S., Smith, K., Sharaf, B., Nicholls, S., Nissen, S., & Anderson, R. (2010). An Intravascular Ultrasound Analysis in Women Experiencing Chest Pain in the Absence of Obstructive Coronary Artery Disease: A Substudy from the National Heart, Lung and Blood Institute-Sponsored Women’s Ischemia Syndrome Evaluation (WISE). Journal of Interventional Cardiology, 23 (6), 511-519.
Maas, A., der Schouw, Y., Regitz-Zagrosek, V., Swahn, E., Appelman, Y., Pasterkamp, G., Cate, H., Nilsson, P., Huisman, M., Stam, H., Eizeman, K., & Stramba-Badiale, M (2010). “Red Alert for Women’s Heart: The Urgent Need for More Research and Knowledge on Cardiovascular Disease in Women.” Proceedings of the European Society for Cardiology Workshop on Gender Differences in Cardiovascular Disease, September 29, Brussels.
Maraka, S., Ospina, N. S., Rodriguez-Gutierrez, R., Davidge-Pitts, C. J., Nippoldt, T. B., Prokop, L. J., & Murad, M. H. (2017). Sex Steroids and Cardiovascular Outcomes in Transgender Individuals: A Systematic Review and Meta-Analysis. The Journal of Clinical Endocrinology & Metabolism, 102 (11), 3914-3923.
von Mering, G., Arant, C., Wessel, T., McGorray, S., Merz, B., Sharaf, B., Smith, K., Olson, M., Johnson, B., Sopko, G., Handberg, E., Pepine, C., & Kerensky, R. (2004). Abnormal Coronary Vasomotion as a Prognostic Indicator of Cardiovascular Events in Women: Results from the National Heart, Lung, and Blood (NHLB) Institute-Sponsored Women’s Ischemia Syndrome Evaluation (WISE). Circulation, 109, 722-725.
Mosca, L., Barrett-Connor, E., & Wenger, N. (2012). Sex/Gender Differences in Cardiovascular Disease Prevention: What a Difference a Decade Makes. Circulation, 124, 2145-2154.
Mosca, L., Benjamin, E., Berra, K., Bezanson, J., Dolor, R., Lloyd-Jones, D., Newby, K., Piña, I., Roger, V., Shaw, L., & Zhao, D. (2011). Effectiveness-Based Guidelines for the Prevention of Cardiovascular Disease in Women 2011 Update: A Guideline from the American Heart Association. Circulation, 123, 1-22.
Nielsen, M. W., Peragine, D., Neilands, T. B., Stefanick, M. L., Ioannidis, J.P.A, Pilote, L., Prochaska, J. J., Cullen, M. R., Einstein, G., Klinge, I., Leblanc, H., Paik, H.Y., Ristvedt, S., Schiebinger, L. (2020). Gender-Related Variables for Health Research.
Nota, N. M., Wiepjes, C. M., de Blok, C. J., Gooren, L. J., Kreukels, B. P., & den Heijer, M. (2019). Occurrence of Acute Cardiovascular Events in Transgender Individuals Receiving Hormone Therapy: Results From a Large Cohort Study. Circulation, 139(11), 1461-1462.
Pelletier, R., Ditto, B., & Pilote, L. (2015). A composite measure of gender and its association with risk factors in patients with premature acute coronary syndrome. Psychosomatic Medicine, 77(5), 517-526.
Pelletier, R., Khan, N. A., Cox, J., Daskalopoulou, S. S., Eisenberg, M. J., Bacon, S. L., … Pilote, L. (2016). Sex Versus Gender-Related Characteristics: Which Predicts Outcome After Acute Coronary Syndrome in the Young?
Journal of the American College of Cardiology 67 (2), 127-135.
Pepine, C., Anderson, R., Sharaf, B., Reis, S., Smith, K., Handberg, E., Johnson, B., Sopko, G., & Bairey Merz, C. (2010). Coronary Microvascular Reactivity to Adenosine Predicts Adverse Outcome in Women Evaluated for Suspected Ischemia: Results from the National Heart, Lung, and Blood Institute (NHLBI) Women’s Ischemia Syndrome Evaluation (WISE) Study. Journal of the American College of Cardiology, 55 (25), 2825-2832.
Peters, S. A., Huxley, R. R., & Woodward, M. (2014). Diabetes as Risk Factor for Incident Coronary Heart Disease in Women Compared with Men: A Systematic Review and Meta-Analysis of 64 Cohorts including 858,507 Individuals and 28,203 Coronary Events. Diabetologia 57 (8), 1542-1551.
Peters, S. A., Huxley, R. R., & Woodward, M. (2013). Smoking as a Risk Factor for Stroke in Women Compared with Men: A Systematic Review and Meta-Analysis of 81 Cohorts, including 3,980,359 Individuals and 42,401 Strokes. Stroke 44 (10), 2821-2828.
Proctor, R. (2011). Golden Holocaust: Origins of the Global Cigarette Catastrophe and the Case for Abolition. Berkeley: University of California Press, 2011.
Robinson, J., Wallace, R., Limacher, M., Ren, H., Cochrane, B., Wassertheil-Smoller, S., Ockene, J., Blanchette, P., & Ko, M. (2008). Cardiovascular Risk in Women with Non-Specific Chest Pain (from the Women’s Health Initiative Hormone Trials). American Journal of Cardiology, 102 (6), 693-699.
Rytz, C. L., Beach, L. B., Saad, N., Dumnaski, S. M., Collister, D., Newbert, A. M., ... & Ahmed, S. B. (2023). Improving the Inclusion of Transgender & Non-Binary Individuals in the Planning, Completion and Mobilization of Cardiovascular Research. American Journal of Physiology-Heart and Circulatory Physiology. 13 Jan. 2023 https://doi.org/10.1152/ajpheart.00494.2022
Scott, P. E., Unger, E. F., Jenkins, M. R., Southworth, M. R., McDowell, T. Y., Geller, R. J., ... & Woodcock, J. (2018). Participation of women in clinical trials supporting FDA approval of cardiovascular drugs. Journal of the American College of Cardiology, 71(18), 1960-1969.
Schafey, O., Eriksen, M., Ross, H., Mackay, J. (2009). The Tobacco Atlas. Atlanta: American Cancer Society.
Shaw, L., Bugiardini, R., & Bairey Merz, C. (2009). Women and Ischemic Heart Disease: Evolving Knowledge. Journal of the American College of Cardiology, 54 (17), 1561-1575.
Stanford Research into the Impact of Tobacco Advertising (SRITA).
World Health Organization (WHO). (2018). Gender-Responsive Tobacco Control.
World Health Organization (WHO). (2010A). WHO Calls for Protection of Women and Girls from Tobacco. Geneva: WHO Press.
World Health Organization (WHO). (2009). Report on the Global Tobacco Epidemic: Implementing Smoke-Free Environments. Geneva: WHO Press.
World Health Organization (WHO). (2008). Causes of Death: 2008 Summary Tables. Geneva: WHO Press.